 Bloat is the term that is often used to describe the condition known in veterinary medicine as Gastric Dilatation-Volvulus (GDV).
Bloat is the term that is often used to describe the condition known in veterinary medicine as Gastric Dilatation-Volvulus (GDV).
This is where a dog's stomach rapidly fills up with gas and rotates or flips over on itself, resulting in the blockage of both the entrance and exit of the stomach.
Stomach bloat is a potentially life-threatening condition for your dog if not recognized and treated early.
As an emergency veterinarian, I have seen countless cases of GDV, some of which have successfully left the hospital post-surgical correction, many of which have not.
If you feel that your dog could be suffering from GDV, get them to an emergency veterinarian right away. Time is of the essence!
If you're not sure whether your dog is bloated, read on and watch the video below. But again, don't delay!
First off, GDV is different than food bloat – where your dog has eaten way too much. If you know or suspect your dog has eaten 2–5 times their normal daily intake, read our food bloat article and get them medical attention.
What Are Some of the Common Symptoms of Dog Bloat?
- Retching (vomiting without producing any vomitus)
- Excessive drooling (may include foamy saliva)
- Panting
- Distended stomach
- Pacing
- Restlessness/Anxiousness
- Crying and/or whining
- Inability or unwillingness to settle or lie down
- Increased heart rate
- Pale mucus membranes (the tissue around their teeth)
- The appearance of a wide stance with elbows extended
Not all dogs with GDV will exhibit all of these signs and symptoms. Even some of the most common symptoms of bloat aren’t easy to spot.
In the most general sense, a “bloated” stomach refers to swelling or distension of the abdomen. If your dog’s stomach appears bloated, it could be due to a number of possible causes, ranging from mild to severe, including pregnancy, heart failure, liver dysfunction, uterine infection ("pyometra"), internal bleeding, as well as GDV, and several others. Most of these are very serious and life-threatening conditions, including GDV. And because of this, it's fair to say that any dog that "looks bloated" should always be taken to the vet ASAP.
The eye-opening video below from the Akita Rescue Mid-Atlantic Coast is so helpful. We are very lucky that they were able to catch such a clear example of GDV/bloat in progress! As you'll see, and as they highlight in the voiceover, the poor dog in the video is exhibiting many of the dog bloat symptoms. Luckily, he was rushed to an emergency vet and survived.
For more detail about each dog bloat symptom and what GDV is, read our dog bloat prevention article.
Questions? To chat with a veterinarian if you suspect your dog has a bloated stomach, Click here
What to Do If You Think Your Dog is Bloated
- Take your dog to a veterinarian for immediate evaluation and treatment. If your regular vet isn't open, seek immediate attention at another veterinary practice or find your closest veterinary emergency hospital.
- Do NOT attempt to treat your dog at home or give your dog any over-the-counter medications, human medications, or other types of “remedy.” This could make matters worse and delay critical treatment.
- Do NOT wait to see if it will pass or improve. It will not. Within 1 to 2 hours, without treatment, a dog suffering from GDV will go into shock. Their heart rate will rise, and their pulse will get weaker, leading to death.
- Call to inform the vet that you’re on your way if it won't unnecessarily delay you getting to the hospital. This will give them time to prepare for your dog’s arrival or redirect you to a nearby facility that is better equipped to give your dog the necessary life-saving treatment.
Prepare for the Outcome
This may be hard to read. But you should also start to have a frank and honest discussion in your head, or with other family members, about your goals for your pet's condition. It is also important to discuss what your time, emotional, and financial resources are and if they will allow you to realize those goals.
Things are going to move very fast once you get to the veterinary hospital, and you'll be asked to make major decisions quickly.
I know this sounds crass and cold, so I'll apologize now, but I would be misleading you and not helping if I didn't tell you that this truly is "gut check" time. Such exploration and discussion are truly in your dog's best interest – as well as yours. You should start getting a sense of "how far you are willing to go" with medical treatment.
Sadly, though understandably, for many people, this often translates into how much money they are willing or able to spend. I know this is sad and that it sucks, but it is the reality. GDV/Bloat isn't just medically devastating; it can also be emotionally and financially devastating, as well. So, it truly is best for you to at least be thinking about these factors before you arrive at the hospital.
Treating GDV is possible, but the outcome isn't. Medical costs can be anywhere between $3,500 and $5,000. If there are complications, it can be $9,000+.
What to Expect When You Arrive at the Veterinary Hospital
- Be ready to move quickly. As GDV is considered a serious emergency, hospital staff will want to take your dog to the back right away for initial diagnostics (X-rays, blood pressure, EKG traces, and more), particularly if you called ahead to notify them of your arrival and suspicions.
You will need to be patient while diagnostics are obtained, but someone will update you as soon as possible. Though that will seem like an eternity to you, please know that the veterinary team is diligently working hard to stabilize your dog and get you the information you need.
1) X-rays are taken to confirm the presence of a dilated, rotated stomach.
2) Blood tests will be performed to determine if there are signs of damage to tissues and other organs resulting in toxins and symptoms of shock.
3) The team will continue to diligently work on your dog, placing intravenous catheters, administering intravenous fluids, pain medications, obtaining blood pressure, EKG readings, etc., while the veterinarian is reading the tests and coming to talk to you about your options. - Know whether you want to resuscitate (perform CPR). If your dog with GDV suffers a cardiac arrest — which is not uncommon — the hospital staff can begin CPR, but they'll need your permission to do so, and they'll need it quickly. So, it is good to know what you’d want to do in advance just in case.
- Paperwork. Upon check-in, there will be forms and paperwork for you to complete. Use the time that your dog is in the back being stabilized and evaluated to complete these steps so that your dog can be entered into the system as efficiently as possible.
How to Treat Dog Bloat
Your dog has been diagnosed with GDV – what happens next? GDV requires surgery to correct, specifically a procedure called "gastropexy." Stomach bloat is a condition your dog will not survive without surgical treatment. If you do not or aren't able to move forward with the surgery, euthanasia is likely the only other option. While devastating, relieving your dog of their suffering is a humane and compassionate thing to do, albeit gut-wrenching.
If treatment progresses, your dog, once stable, will need to go to surgery to derotate the stomach into its normal anatomic location. At the same time, the health of the stomach wall, spleen, and other organs and intestines will be evaluated. As with any surgery, complications can arise. Your veterinarian will be sure to discuss these with you.
Gastropexy Surgery
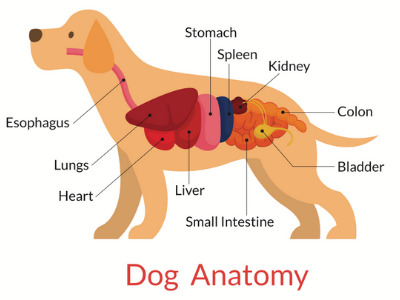 During a gastropexy (or "pexy" for short), the stomach is surgically "tacked" or sewn to the inner surface of your dog's abdominal body wall, the idea being to make a permanent adhesion that will ultimately prevent a future episode of torsion.
During a gastropexy (or "pexy" for short), the stomach is surgically "tacked" or sewn to the inner surface of your dog's abdominal body wall, the idea being to make a permanent adhesion that will ultimately prevent a future episode of torsion.
You should be aware, however, that a stomach that has been tacked can still bloat or dilate; it just can't rotate or torse. It must be noted, however, there have been the occasional cases where tacking has failed and GDV has recurred, though these cases are rare.
This surgery may involve a splenectomy in some cases. A splenectomy (complete removal of the spleen) may be performed in some instances of GDV. The reason for this is that in some cases, the spleen may also get ‘caught up’ and rotate with the stomach when it flips over.
This results in a compromise to the blood supply of the spleen and to the tissues of the spleen itself. A dog can survive perfectly fine without a spleen but not with a spleen that is dying or compromised.
A gastropexy can be done as a preventative surgery. If you have a dog that is predisposed to GDV, for example, if they're a barrel-chested breed, then you may want to consider this procedure as a preemptive move.
If your dog isn't spayed or neutered yet, you may want to consider scheduling this procedure at the same time while they're under anesthesia. Don't hesitate to discuss this with your veterinarian. Read our article on bloat prevention for more ways to help avoid this devastating condition from happening.
Is surgery the only option?
The short answer. Yes. The only appropriate treatment for GDV is surgical correction. A dog’s stomach may be able to be decompressed by a veterinarian by passing a tube through the mouth, and in some cases, this may result in the derotation of the stomach. However, this does not mean that the issue has been solved, and your dog can now go home.
DO NOT EVER ATTEMPT TO DECOMPRESS THE STOMACH AT HOME UNDER ANY CIRCUMSTANCES. It could result in putting a tube in your dog's lungs and killing or severely injuring your dog, or getting injured from a dog bite. This procedure must be done by a veterinary medical professional.
If my dog’s stomach is decompressed by the veterinarian, why is surgery still likely needed?
As mentioned above, the stomach’s blood supply will have been compromised, likely for several hours. The stomach tissue itself needs to be assessed to ensure that it is healthy and the tissue is not dead (necrotic) or dying. And the only way this can be done is by physical assessment and visualization, thus, via surgery.
Additionally, your dog will still be experiencing the effects of shock. So they will need to stay in the hospital for a while. This is not going to automatically improve once a stomach is decompressed or derotated. The toxins and damaging effects the various physiologic systems in your dog’s body took while they were experiencing GDV will take a significant period of time to correct. Intravenous fluids, medications, and skilled monitoring are needed to immediately recognize and correct any abnormalities or imbalances noted while your dog is hospitalized.
You Cannot Treat GDV at Home
You 100% cannot and should not attempt to treat GDV at home. Even in the ‘early stages’ of GDV. There are no home remedies, medications, or supplements that are safe or effective to give a dog that is suffering from GDV/Bloat. No amount of Gas-X® or any other at-home or over-the-counter treatment will cure or help a dog or prevent GDV from developing.
In fact, the struggle of trying to get oral medications into a dog when they have a potentially twisted stomach may worsen their discomfort and distress. It delays treatment and also carries the risk that the medication will wind up going down their trachea and into their lungs or that you could be bitten.
The only correct way to treat bloat is to get your dog to a veterinarian as soon as possible! Even if it turns out not to be a case of GDV, you and your dog will be happier for the peace of mind and relief a veterinary evaluation can provide.
The time wasted trying to give at-home treatments will unnecessarily delay the proper veterinary evaluation and care needed to give your dog the best chance of survival. Within 1 to 2 hours, without treatment, your dog will go into shock if they're suffering from GDV.
For $5, you can connect with a veterinarian to discuss your dog’s stomach issue.
Connect now
Rates may differ for those residing outside the U.S. You'll have access to a vet for 7 days.
What to Do After Your Dog Comes Home From the Hospital
Your veterinarian will provide you with care instructions to follow at home. Here are some things to be mindful of.
-
Prepare a small, confined space. It's absolutely critical for your dog's healing process their movements and activity be limited following GDV surgery. Prepare a crate or small pen for them at home. You can get some ideas in our How to Set Up a Safe Space for Your Dog article.
-
Watch for post-surgery complications such as infection, inflammation, lack of appetite, vomiting, and pain. Complications can arise days or even weeks after surgery. If your dog is acting abnormally, or if you're otherwise concerned following GDV surgery, don't hesitate to contact your veterinarian or the hospital where the surgery was performed. Do not provide pain medications without discussing it with your doctor. Human pain medication can be toxic for dogs, and if given, must be under the direct supervision of their veterinarian.
- Your dog will likely have a decreased appetite as a result of surgery. However, don’t be alarmed. Feeding small bland meals that are gentle on the gastrointestinal tract, such as boiled chicken breast (no skin, no bones, no salt, or other additives in the water) and white rice to entice them to eat, is a good place to start. Once they start eating small amounts, you can start increasing how much you’re feeding and mixing in their regular diet. It may take a few days for them to return to a normal appetite.
Can Dogs Survive Bloat / GDV?
Dogs suffering from GDV can be saved!
While the Akita Rescue video featured above in this article is an important resource, I would like to clarify one of the statements they make at the end of the video. They say that "bloat is 95% fatal.” It’s very important to note that this quoted mortality rate (i.e., the percentage of affected dogs that die or are euthanized) is for cases that go undetected and/or where appropriate treatment is declined or unnecessarily delayed.
The prognosis for survival is significantly better for cases that are (1) caught earlier and (2) treated appropriately and promptly. Survival rates for dogs treated appropriately and promptly have been reported as high as 85%. It also has to be mentioned that many dogs are humanely euthanized in this condition due to finances, age of the pet, and other reasons such as comorbidities (other health issues), which are not taken into account when calculating the percentage of survival rates.
If recognized and treated aggressively and early, the survival rate is much more favorable.
Play It Safe
Still unsure if your dog has GDV? Even if you think there’s a chance that your dog may currently be suffering from this condition, it is recommended you err on the side of caution and take them for immediate veterinary evaluation. The cost of an emergency vet visit will pale in comparison to the peace of mind you’ll get by doing so. Or the cost of your dog’s life.
Below are some of the comments we've received by email or on our website from people who were thankful they took our advice. Good luck! We hope the best for you and your dog.

Sign up for our twice-monthly Paws & Play newsletter for life-saving tips!




